Have you ever experienced abdominal pain so sharp that you can’t move for fear of sending your body into spasms? This could be a symptom of pancreatitis, and you need to address it.
What Does the Pancreas Do?
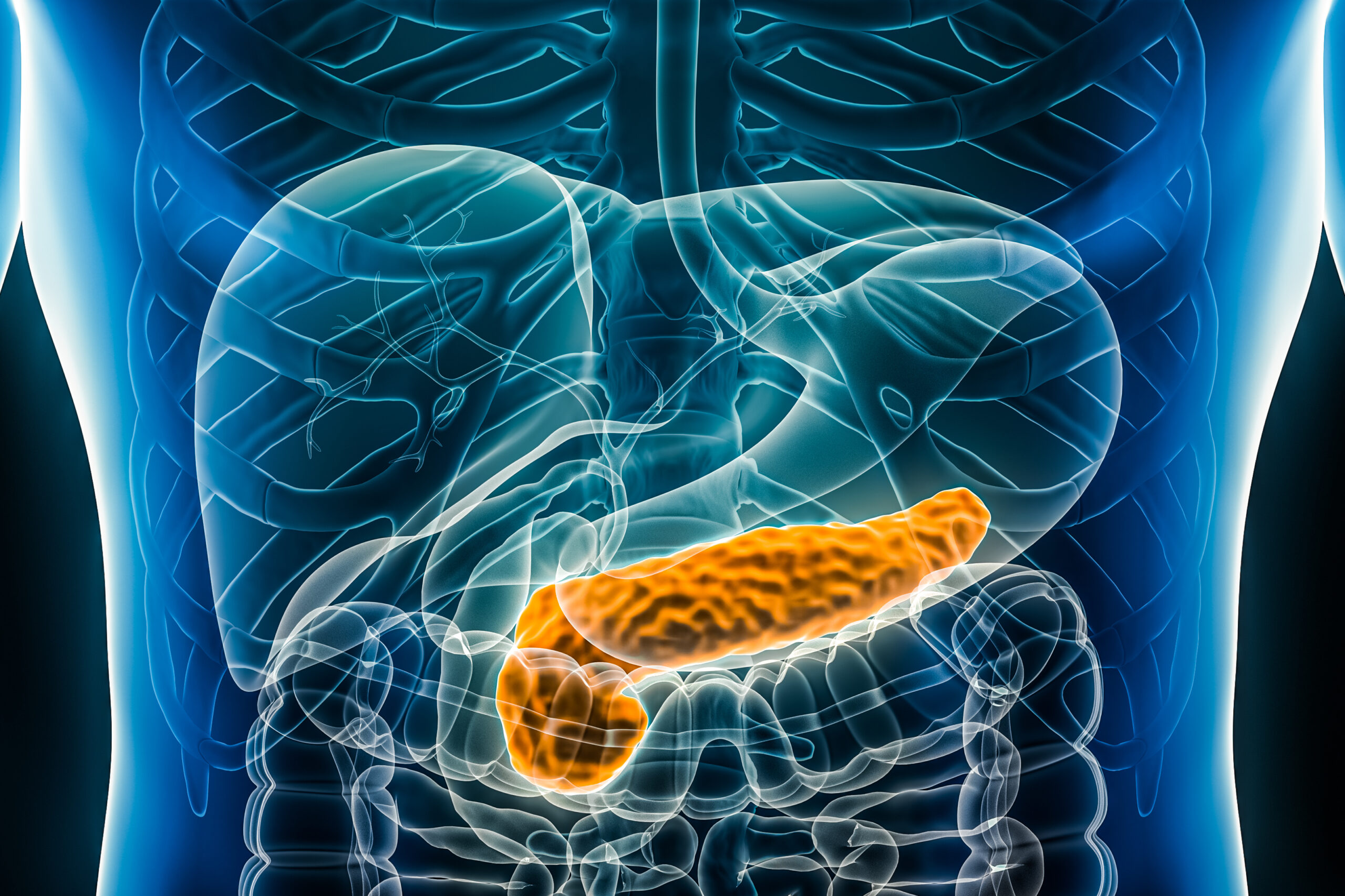
The pancreas is a small organ located behind the stomach, and it plays a crucial role in digestion and blood sugar regulation. It produces enzymes that help break down food in the small intestine and hormones like insulin and glucagon that control blood sugar levels. Inflammation of the pancreas can disrupt these functions and lead to serious health issues.
The Fear of Pancreatitis
Pancreatitis, an inflammation of the pancreas, instills a deep sense of fear and apprehension among those familiar with its symptoms and potential complications. This fear is not unwarranted, as the condition can escalate quickly, leading to severe health dilemmas, including chronic pain, diabetes, and even pancreatic cancer.
The unpredictable nature of pancreatitis, where flare-ups can occur without warning, significantly impacts the quality of life of sufferers, causing both physical discomfort and emotional distress.
Acute Pancreatitis
Acute pancreatitis is characterized by the sudden onset of severe abdominal pain due to pancreas inflammation. Triggered most commonly by gallstones or excessive alcohol consumption, this condition results in a variety of symptoms, including nausea, vomiting, fever, and a rapid heartbeat.
Immediate medical attention is crucial to manage the symptoms and prevent complications, as the inflammation can cause tissue damage and infection and even lead to organ failure if left untreated.
Managing acute pancreatitis often involves hospitalization, where patients may receive fluids intravenously, pain relief, and sometimes, procedures to remove blockages causing the inflammation.
Chronic Pancreatitis
Chronic pancreatitis is a long-term condition where the inflammation of the pancreas persists over many years, leading to permanent damage. Unlike acute pancreatitis, which can resolve with treatment, chronic pancreatitis often develops slowly and can be the result of repeated episodes of acute pancreatitis.
It is frequently associated with factors like long-term alcohol abuse, genetic conditions, and certain autoimmune disorders. Symptoms can include persistent abdominal pain, weight loss due to malabsorption of nutrients, and the development of diabetes as the insulin-producing cells are damaged.
The management of chronic pancreatitis focuses on pain relief, dietary changes to support digestion, and enzyme supplements to aid in food breakdown.
Causes of Pancreatitis
Pancreatitis can be triggered by a variety of factors, with the most common being gallstones and excessive alcohol consumption. Gallstones can block the duct through which the pancreatic enzymes exit, causing these enzymes to attack the pancreas itself.
Similarly, excessive alcohol intake leads to the production of toxic substances that can inflame the pancreas. Other potential causes include certain medications, high levels of triglycerides in the blood, autoimmune diseases, and genetic predispositions.
In some cases, the exact cause of pancreatitis may remain unknown, classified as idiopathic pancreatitis. Recognizing and mitigating the risk factors associated with pancreatitis is crucial for preventing and managing the condition.
Catching and Preventing
As stated previously, recognizing and mitigating the risk factors for pancreatitis is vital in preventing the onset of this condition. A primary step involves thoroughly understanding one’s health and lifestyle choices.
Regular medical check-ups: This can identify issues like high triglyceride levels or the presence of gallstones early on.
Adopting a balanced diet: Watching and tracking your food consumption is always a great action when preventing conditions.
Limiting harmful habits: Habits like alcohol consumption or tobacco use should be limited if not eliminated.
Engage in regular exercise: Regular physical activity can help maintain healthy levels of triglycerides and reduce the risk of developing gallstones. Obesity is a risk factor for pancreatitis, so maintaining a healthy weight through diet and exercise can significantly lower your chances of developing the condition.
Be aware of family history: If you have a family history of pancreatitis, it is essential to inform your doctor and monitor your health closely.
Track concerning medical conditions: Certain conditions, such as autoimmune disorders or diabetes, can increase your risk of developing pancreatitis. Maintaining these conditions through proper treatment and lifestyle changes can help prevent complications.
Inflammation: A Warning Sign
Inflammation is the body’s response to injury or infection, but chronic inflammation can indicate an underlying health issue. Paying attention to symptoms like persistent abdominal pain, particularly after eating fatty foods or drinking alcohol, nausea, and weight loss can help catch pancreatitis in its early stages.
If you experience these symptoms, seek medical attention promptly to address the issue and potentially prevent more severe complications. By recognizing warning signs and making necessary lifestyle changes, we can work towards avoiding pancreatitis and living a healthier life.
When Do You Ask a Doctor?
If you experience persistent abdominal pain or any other symptoms associated with pancreatitis, it is essential to seek medical attention promptly. While some cases of acute pancreatitis resolve with treatment, others can lead to serious complications if left untreated.
To learn more, contact your healthcare provider as soon as possible or set up an appointment with the GI Specialists at Gastro Florida.


 Close
Close